Inabiliaty to Walk Again After Codeine Overdose
Non-Fatal Opioid Overdose and Associated Health Outcomes: Final Summary Study
Jon Zibbell, PhD, Jennifer Howard, PhD, Sarah Duhart Clarke, BS, Abigail Ferrell, BA, and Sarita L. Karon, PhD
RTI International
September 2019
Printer Friendly Version in PDF Format (33 PDF pages)
Abstract
Non-fatal opioid overdose (NFOO) is a significant crusade of opioid-related morbidity in the United States. Equally the number of NFOOs continues to grow, it is of import to understand the short- and long-term consequences of NFOO. This report examines the existing literature on the astute and chronic wellness and functional outcomes of individuals who feel NFOO, and also identifies differences in outcomes for NFOOs involving illicitly-manufactured fentanyl.
This report was prepared under contract #HHSP233201600021I betwixt HHS'due south ASPE/DALTCP and Research Triangle Institute. For additional information almost this subject field, y'all can visit the DALTCP home page at https://aspe.hhs.gov/function-disability-aging-and-long-term-care-policy-daltcp or contact the ASPE Project Officers, Daniel Schwartz, DEB Potter and Helen Lamont, at HHS/ASPE/DALTCP, Room 424E, H.H. Humphrey Building, 200 Independence Avenue, Southward.W., Washington, D.C. 20201; Daniel.Schwartz@hhs.gov.
DISCLAIMER: The opinions and views expressed in this report are those of the authors. They do not reflect the views of the Department of Health and Human Services, the contractor or whatsoever other funding system. This report was completed and submitted on March 4, 2019.
Table OF CONTENTS
ACRONYMS
EXECUTIVE SUMMARY
ane. BACKGROUND
2. Information AND METHODS
2.i. Scoping Review Framework
2.2. Identification of Relevant Publications
2.3. Choice of Publications
ii.4. Information Extraction and Synthesis
three. RESULTS
iii.1. Furnishings of Non-fatal, Opioid-Involved Overdoses
3.2. Differing Health Outcomes between Illicitly-Manufactured Fentanyl, Heroin, and Prescription Opioids
3.iii. Interaction between Pre-existing Conditions and Subsequent Overdose
three.4. Health Service Utilization
4. Give-and-take
4.1. Discussion of Results
4.2. Gaps in the Literature
4.3. Importance of Information
4.4. Study Limitations
five. Determination
REFERENCES
APPENDIX A: Example Search Strategy--PubMed
NOTES
List OF FIGURES
- Figure i: Publication Selection Process
List OF TABLES
- TABLE 1: Search Terms
ACRONYMS
The following acronyms are mentioned in this written report and/or appendix.
| ASPE | Function of the Assistant Secretary for Planning and Evaluation |
|---|---|
| CDC | Centers for Disease Control and Prevention |
| CNS | Central Nervous Arrangement |
| DEA | Drug Enforcement Administration |
| International monetary fund | Illicitly-Manufactured Fentanyl |
| MMWR | Morbidity and Mortality Weekly Report |
| MOR | µ-Opioid Receptor |
| MPTP | Illicitly-Manufactured Meperidine (ane-methyl-4-phenyl-1,2,3,6-tetrahydropyridine) |
| MRI | Magnetic Resonance Imaging |
| NFOO | Non-Fatal Opioid-involved Overdose |
| NIH | National Institutes of Health |
| OIRD | Opioid-Induced Respiratory Depression |
| RTI | Enquiry Triangle Establish |
| SAMHSA | Substance Corruption and Mental Health Services Assistants |
EXECUTIVE SUMMARY
The Office of the Assistant Secretary for Planning and Evaluation (ASPE) contracted with RTI International to conduct a scoping review of the scientific literature on non-fatal opioid-involved overdose (NFOO) to better understand the health outcomes and health care implications associated with opioid epidemic. NFOO is a significant cause of opioid-related morbidity in the United states, and is of heightened interest to ASPE given the sharp increase in fatal and non-fatal opioid overdoses equally a event of the current fentanyl crisis. Compared to the starting time and 2d phases of the opioid epidemic, when the majority of opioid-related morbidity and mortality was associated first with prescription opioids and then with heroin, illicitly-manufactured fentanyl (IMF) is now the leading cause of fatal opioid overdoses (CDC, 2017; O'Donnell, Gladden, & Seth, 2017). People who consume IMF, either wittingly or unwittingly, are at higher take chances for adventitious overdose, feel comparatively atypical overdose-related side furnishings, have unique risk profiles, and are at higher take chances for poorer health outcomes (Somerville, 2017). To our noesis, no investigation has been conducted to examine whether the sharp increase in NFOOs over the last several decades is negatively impacting overdose victims' chronic physical and mental health outcomes. To investigate the status of the scientific literature regarding the consequences of NFOO on victims' concrete and mental health, nosotros conducted a scoping review of the existing noesis in multiple stages: (ane) publication identification; (2) selection of publications; and (iii) data extraction, charting, and synthesis. Key findings from our review are presented below.
Key Findings
Findings from this scoping review ostend that NFOO is an important cause of morbidity amidst persons who misuse and abuse prescription and/or illicitly-manufactured opioids (due east.k., heroin). The findings are summarily presented beneath and organized by three topics: (ane) health outcomes associated with NFOO; (2) differing health outcomes for NFOOs that involve prescription opioids vs. heroin vs. IMF; and (3) the interaction between overdose victims' pre-existing health conditions and the wellness outcomes associated with NFOO.
Health Consequences of Not-Fatal Opioid-involved Overdoses
Opioid-Induced Respiratory Depression
Opioid-induced respiratory depression (OIRD) was identified as a master complication and the nigh dangerous source of adverse health outcomes associated with NFOO (Male monarch, Morris & Schahmann, 2015). The health consequences associated with OIRD include a range of acute complications that develop during or immediately later a NFOO effect. OIRD most oft presents as acute respiratory compromise with victims reverting to normal animate action either on their own or with the use of an opioid overdose reversal drug like naloxone (Wermeling, 2015). Near NFOO victims recover from OIRD and present only minor health consequences (e.grand., dizziness, defoliation, ineptness) lasting minutes to hours (Sporer & Dorn, 2001; Buajordet et al., 2004; Olfson et al., 2018).
Brain Injury
Most literature identifying chronic complications associated with NFOO concerns the evolution of hypoxia-related brain injuries and subsequent complications caused by a prolonged version of OIRD that contributes to a protracted deficiency of oxygen reaching the body's tissues (Ueno et al., 2018; Somerville et al., 2017; Betts, Ritter, & Kubal, 2012; Salazar & Dubow, 2012). The range of health complications associated with opioid-induced hypoxia includes kidney failure, heart complications, neurologic consequences, seizures, nerve impairment, temporary motor paralysis, fluid buildup in the lungs, stroke, and pneumonia from inhaling vomitus (Marino et al., 2018; Betts, Ritter & Kubal, 2012; O'Brien & Todd, 2009; Fitzgerald et al., 2000).
Several studies have employed encephalon scans and demonstrate susceptibility of certain regions of the brain to hypoxic injury, with short-term retentivity loss and changes in cerebral and physical performance documented. Stroke has also been observed in rare NFOO cases. Opioid-induced hypoxic encephalon injury has too been shown to contribute to the development of astringent disability, including mental disorientation, the loss of body motion, gait changes, incontinence, paralysis of lower extremities, and changes in beliefs due to altered mental states, among a range of other presentations (Buttner et al., 2000). Slower reaction fourth dimension, impaired memory (amnestic syndrome), reduced motor skills, and diminished physical operation have all been documented every bit hypoxic-related brain injuries associated with NFOO (Barash, Somerville, & DeMaria, 2017; Ueno, et al. 2018; Somerville et al., 2017; Betts, Ritter, & Kubal, 2012; Salazar & Dubow, 2012).
Differences in Effects of Overdoses between Single, Multiple, and Recurring Opioid Overdose
There is relatively scarce literature detailing with health outcomes that develop among victims who feel more than 1 NFOO. However, one study demonstrated increased risk for hypoxic encephalon damage among persons who feel multiple or recurring opioid overdose events due to repeated and prolonged hypoxia (Zamora et al., 2015).
Differing Wellness Outcomes between Illicitly-Manufactured Fentanyl, Heroin, and Prescription Opioids
Fentanyl, a constructed opioid 100 times more stiff than morphine, stands apart from heroin and other semi-synthetic opioids in these findings by its relatively high potency and rapid onset of action when smoked, sniffed, or injected. These characteristics are the event of fentanyl's high lipid profile, which allows its molecules to deliquesce speedily in fats and rapidly cantankerous the claret-brain barrier (Burns et al., 2016). A rapidly growing supply of International monetary fund in existing heroin markets has substantially increased the number of fentanyl overdose deaths over the last 5 years, with fentanyl deaths surpassing the number of deaths from both heroin and prescription opioids in 2022 and 2017. All the same, few studies have examined the specific wellness complications associated with fentanyl overdose compared to overdoses involving prescription opioids or heroin. The medical research literature does identify several side effects resulting from the clinical use of intravenous fentanyl in hospital settings, with skeletal muscle rigidity and breast wall rigidity the near unremarkably reported (Burns et al., 2016). Chest wall rigidity, colloquially referred to as "wooden chest syndrome," is understood every bit the acute inability to ventilate or move the breast wall; this effect poses serious complications for ventilating overdose victims suffering from OIRD in non-hospital settings.
Interaction between Pre-existing Weather condition and Subsequent Overdose
Few studies included in our review examined the interplay betwixt pre-existing physical or mental health weather condition among people consuming opioids and subsequent NFOO amid this population. Some mental health conditions, such equally depression and suicidality, accept been strongly associated with opioid utilise disorder and drug overdose. Comorbid mental health conditions are identified every bit risk factors for drug overdose, but it is difficult to distinguish the degree to which they are influenced or exacerbated by NFOO in retrospective studies (Neale, 2000). Beyond depression, suicide attempts are shown to exist associated with unintentional overdose (Neale, 2000; Bradvick et al., 2007), and suicide risk is correlated with higher numbers of drug overdoses amongst victims (Bradvick et al., 2007). It is unclear, even so, to what degree suicidality is exacerbated by drug overdose and vice versa. Symptoms resulting from opioid-induced hypoxia described above may exacerbate pre-existing disabilities and weather condition among NFOO victims. For case, declines in a person'south cognitive and physical functioning due to having one or more NFOO may present difficulties for managing their existing chronic illnesses, such as diabetes, addiction, or clinical depression (King, 2015).
Discussion and Decision
As the number of NFOO continues to grow, information technology is paramount that health care and treatment providers as well as policymakers have information on how NFOO tin can impact overdose victims' mental and concrete performance in both the curt-term and long-term. This is specially truthful for the population of people who swallow street opioids, given their increased risk for fentanyl consumption. Without this data, providers and policymakers will be hindered in their ability to provide appropriate and high-quality health care and supportive services for overdose victims. Further, they will be providing care to this population with no real understanding or guidance for how to identify the longer-term health consequences that may derive from recurring hypoxic overdose events, especially those associated with Imf use.
The purpose of this scoping review was to better understand the wellness and functional outcomes associated with NFOO. Afterward reviewing 48 peer-reviewed and greyness publications identified and selected for review, our analysis concluded that numerous clinical complications are associated with NFOO. Among these, nearly of the concentration focuses on acute outcomes stemming from respiratory low and hypoxia. The current lack of longitudinal studies examining the chronic complications resulting from non-fatal opioid overdose events restricts our power to understand the longer-term furnishings of opioid overdose on victims' physical, mental, and cognitive functioning. Most critical are the downstream effects of a fentanyl overdose crisis that, betwixt 2022 and 2017, killed males aged 25-44 at an age-adjusted rate of 27 per 100,000. The fentanyl crisis has contributed to a population of fentanyl consumers who overdose with more than frequency than they did with prescription opioids or heroin because of fentanyl'south college potency and more rapid duration of activeness.
Potentially fruitful avenues for future research include an boosted review of the literature with expanded search strategies, the collection of primary data through interviews with key subject thing experts and NFOO victims, and longitudinal studies utilizing secondary data. A longer-term recommendation for clinical research may include expanding current encephalon injury studies, such as the Chronic Traumatic Encephalopathy program at Boston University, to include fatal overdose victims who experienced recurring not-fatal hypoxic overdose events prior to death.
1. BACKGROUND
The opioid epidemic in the U.s.a. continues to generate unprecedented levels of morbidity and bloodshed. More than than 70,237 people died from a drug overdose in 2017, and over two-thirds of those deaths involved an opioid (CDC, 2017). The rise in overdose deaths since 2013 has been largely owing to the introduction of fentanyl (a constructed opioid nearly 50 times more potent by weight than heroin) inside illicit drug supplies. Illicitly-manufactured fentanyls (IMFs)[1] typically enter the state via illicit drug channels aslope heroin and other illicit drugs, earlier being sold either by itself or mixed with heroin (DEA, 2017). IMFs have as well been distributed in the form of counterfeit prescription drugs, such every bit OxyContin or Xanax, which accept been linked to overdose outbreaks in multiple states (Green & Gilbert, 2016).Since 2016, prescription opioid-involved overdose deaths have been failing, and deaths from heroin and IMFs are at present the main drivers of opioid-related mortality (O'Donnell, Gladden, & Seth, 2017), with IMFs responsible for a majority of opioid overdose deaths since 2022 (CDC, 2017). According to the Centers for Disease Control and Prevention's National Syndromic Surveillance Program, opioid overdose emergency department visits increased roughly 30% from third quarter 2022 (July-September) to third quarter 2022 in all five Usa regions--the Midwest showed the greatest increase (69.7%), followed past the West (xl.3%), Northeast (21.3%), Southwest (20.ii%), and Southeast (14.0%) (CDC, 2018). The increases in opioid overdose rates are consequent with previous reports indicating that non-fatal overdose hospitalizations and emergency department visits associated with heroin and IMF poisonings are on the rise (CDC, 2017).
Opioid abuse and non-fatal opioid overdose have been linked to concurrent upsurges in overdose-related health complications. For case, a 2022 written report in Journal of the American Board of Family Medicine documented increases in agin health outcomes associated with increased duration of opioid apply (Paulozzi et al., 2014), and the National Institutes of Health (NIH) have linked opioid poisoning with hypoxia-related complications such as organ organisation damage, cardiac arrest, stroke, psychosis, and death (NIH, n.d.). The current IMF crisis has contributed essentially to the sharp increase in fatal and non-fatal opioid overdose, with Imf contributing to the evolution of unusual non-fatal overdose presentations. For example, a recent example written report from Register of Internal Medicine identified increases in unusual amnestic syndrome associated with the combined use of International monetary fund and cocaine (Duru et al., 2018).
Similarly, increases in anecdotal reports in the U.s. take identified increases in previously unseen side furnishings associated with Imf-involved overdoses, such as rigid breast syndrome, acute rigor mortis, and memory loss (Burns, 2016). People who utilise heroin and International monetary fund are at higher risk for recurring overdose, they experience unusual overdose-related side effects, and they have unique health concerns or are at higher chance of poorer health outcomes (Somerville, 2017). Taken together, the increment in both known and unfamiliar/unusual health outcomes associated with opioid poisoning, and specifically IMF-involved overdose, suggests the need for a rigorous review of the literature to investigate existing scientific knowledge on the short and long-term effects of non-fatal opioid overdose, with a specific focus on Imf and heroin.
The Part of the Assistant Secretarial assistant for Planning and Evaluation (ASPE) contracted with RTI International to conduct a scoping review to better sympathize the health and functional outcomes implications associated with non-fatal opioid-involved overdose (NFOO). This study addressed the following research questions:
-
What effects exercise non-fatal, opioid-involved overdoses have on overdose victims' concrete and mental health, including simply not express to functional and cognitive harm?
-
How exercise physical and mental health outcomes, including but not limited to functional and cognitive damage, associated with non-fatal, opioid overdoses that involve Imf and fentanyl analogs (eastward.g., acetylfentanyl, furanylfentanyl, carfentanil, etc.) differ from the physical and mental wellness outcomes of non-fatal overdoses involving heroin and other semi-synthetic opioids (e.g., oxycodone)?
-
How do non-fatal overdoses interconnect with or exacerbate other concrete weather condition and health outcomes among overdose victims, such every bit memory loss, cerebral impairment, mental illness, and increased physical disability?
two. DATA AND METHODS
2.i. Scoping Review Framework
Our methods were guided by a framework for conducting scoping reviews originally proposed by Arksey & O'Malley (2005) and afterward expanded by Levac & colleagues (2010; Colquhoun et al., 2014). This section describes the steps nosotros undertook to ensure that we explored the full breadth of the literature and obtained comprehensive information nigh the short-term and long-term outcomes of non-fatal overdoses.
2.two. Identification of Relevant Publications
We began this scoping review past creating a data charting tool to capture and organize the information identified during the form of the review. We designed our tool (i.e., an Excel database) to capture:
-
Publication information, including author(s) names, study title, publishing journal or arrangement/agency, publication year, and abstract.
-
Reviewer initials, reviewers' determinations for including or excluding a publication during each step of the review, and reasons for exclusion at each footstep.
-
Report data extracted during the review process, such as study drug of focus, methodology, and findings.
The data charting tool immune reviewers to synthesize information past research question and subquestion/theme and provide additional notations that may be pertinent as, "additional notes/noteworthy findings." In add-on, the tool immune reviewers to indicate key articles and boosted databases noted in the reviewed publication that were further investigated for possible inclusion in the review.
After creating a charting tool, we took a two-role approach to place relevant studies for inclusion in the review: we conducted a structured search of academic literature and a thorough review of several grayness literature sources. The two searches were composed of multiple steps that included developing preliminary lists of search terms, exclusion and inclusion criteria, and databases and organizational and agency websites for conducting the searches. Tabular array one shows the organizations, agencies, and publications searched every bit well as the search terms used.
| Table i. Search Terms | |
|---|---|
| Peer-Reviewed Literature | Grey Literature |
| 1998-present English language Databases: PubMed, Embase, Web of Science, PsycINFO, Toxline, ScienceDirect, JSTOR, Google Scholar Search Terms (for starting time search): opioid* OR fentanyl OR "illicitly-manufactured fentanyl" OR "illicitly-made fentanyl" OR acetylfentanyl OR furanylfentanyl OR carfentanil OR heroin OR oxycodone OR oxymorphone OR Opana OR hydromorphone OR Dilaudid OR OxyContin OR hydrocodone OR Vicodin OR "novel psychoactive substance*" OR methadone AND overdos* AND ("non-fatal" OR nonfatal OR unintentional* OR accidental* OR accident) Search Terms (for second search): opioid* OR fentanyl OR "illicitly-manufactured fentanyl" OR "illicitly-made fentanyl" OR acetylfentanyl OR furanylfentanyl OR carfentanil OR heroin OR oxycodone OR oxymorphone OR Opana OR hydromorphone OR Dilaudid OR OxyContin OR hydrocodone OR Vicodin OR "novel psychoactive substance*" OR methadone AND overdos* OR postoverdos* AND hypoxic hypoxia OR arterial hypoxia Search Terms (for third search): opioid* OR fentanyl OR "illicitly-manufactured fentanyl" OR "illicitly-made fentanyl" OR acetylfentanyl OR furanylfentanyl OR carfentanil OR heroin OR oxycodone OR oxymorphone OR Opana OR hydromorphone OR Dilaudid OR OxyContin OR hydrocodone OR Vicodin OR "novel psychoactive substance*" OR methadone AND overdos* OR postoverdos* AND (longitudinal OR follow-upwards) AND (intervention* OR medication assisted handling*) | 1998-present English language Organizations/Agencies:
Inquiry Institutes:
Search terms: opioid OR fentanyl OR acetylfentanyl OR furanylfentanyl OR carfentanil OR heroin OR oxycodone OR oxymorphone OR Opana OR hydromorphone OR Dilaudid OR OxyContin OR hydrocodone OR Vicodin OR methadone AND Overdose OR Nonfatal |
Our team worked with an experienced librarian to refine the approach to identifying relevant studies at multiple points in the process. An example search strategy tin can be establish in Appendix A .
Once we identified a list of initial studies, nosotros downloaded the publications into an Endnote database, removed duplicate publications, and completed a high-level review of the resulting publication titles. Our team met with the librarian to discuss the initial results and refined the exclusion and inclusion criteria to focus the scope to identify relevant studies. We paid special attending to ensure that all relevant systematic reviews were adequately captured. This step was completed three times to ensure all relevant peer-reviewed publications were captured. One time we agreed that all relevant studies were identified from all relevant sources, a team fellow member imported the publication data and abstracts from selected relevant publications into the data charting tool.
Concurrent to this review, members of the research team completed a search of the grey literature. They identified major organizations and governmental agencies and used key search terms to place relevant resource from the website of each organization and agency. All resources identified from the search of the greyness literature were included in the data charting tool for boosted review.
2.iii. Selection of Publications
Later on contained review by two members of the research team, we selected studies for inclusion. The purpose of the abstruse review was ii-fold: (a) to further refine the inclusion/exclusion criteria; and (b) to begin the process of eliminating studies from further assay. A third, senior reviewer was included every bit a "tie breaker" in the instances where there was disagreement between the reviewers. Only those publications that both reviewers indicated should be included were reviewed farther. A reason for exclusion was included for all publications excluded from further analysis.
Ii independent reviewers from the research team then assessed each article selected for inclusion. Like the abstract review, this cess served two purposes: to further narrow the studies included in the review (i.e., remove studies that were not relevant to the three research questions) and to extract information using a qualitative thematic analysis arroyo. We focused on the findings of the publications, merely also summarized content from other sections of the publications that were helpful in answering the research questions or providing information on other relevant studies.
During each level of the review, nosotros evaluated the quality of the resource identified and excluded resources that did non have the necessary methodological rigor for the review. We evaluated quality based on the number or type of citations (e.thousand., publications without citations were excluded) included in the publication equally well every bit a minimum level of detail in the publication (e.grand., conference proceedings without detailed notes and citations were excluded).
We identified 254 articles through a search of the peer-reviewed and grey literature. 1 hundred and eight of these were reviewed in full for relevance; 60 of that 108 were culled based on decision that the publication type equally unsuitable (six), the report focused on a substance not included in the inquiry questions (iv), or they were otherwise not relevant (50). Data was extracted and synthesized from the 48 publications that met our inclusion/exclusion criteria. See Figure 1 .
| FIGURE one. Publication Selection Process |
|---|
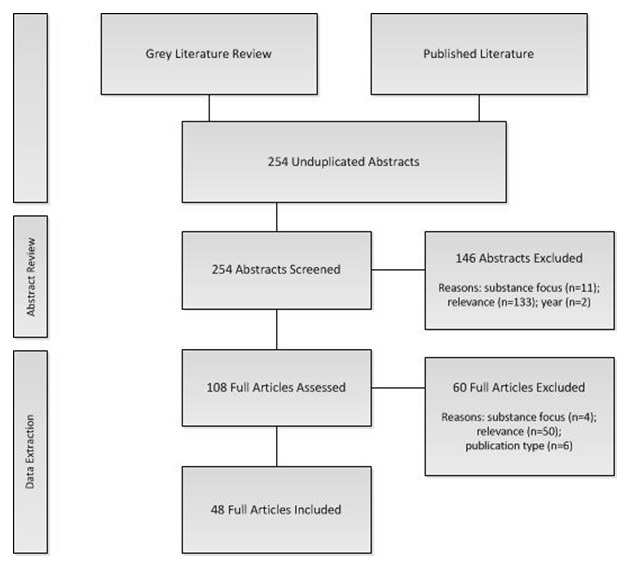 |
2.4. Information Extraction, Charting and Synthesis
Once relevant publications were selected for inclusion, we began extracting content relevant to each of the research questions and charting the information in the data charting tool. We and then synthesized the data. To synthesize the data collected from the publications, we conducted a qualitative thematic analysis. This was done by identifying themes and subthemes within the content extracted by inquiry question. Themes and subthemes identified were then documented in the data collection tool for further analysis and synthesis. We completed an additional analysis of the themes and subthemes identified across the three research questions to contextualize the implications of the results for wellness care do. Finally, we identified gaps in the literature examined in order to highlight time to come research needs.
3. RESULTS
3.i. Effects of Not-Fatal Opioid-Involved Overdoses
Many of the studies included in this review focus on the health effects associated with NFOO. Findings ostend that non-fatal overdoses involving µ-receptor opioids (including natural, semi-synthetic and constructed opioids) is an important cause of morbidity amid persons who misuse and abuse prescription and/or illicitly-manufactured opioids (e.1000., heroin). NFOO is of clinical consequence due to its association with a wide range of acute and chronic medical complications, including aspiration pneumonia,[2] pulmonary edema,[3] bronchopneumonia,[4] rhabdomyolysis,[five] muscle tissue breakup, hypoxic brain injury, peripheral neuropathy,[six] renal failure, cerebral damage, and traumatic injuries sustained during overdose (Darke & Hall, 2003; Ridgway & Pountney, 2007). One report found more than 3-quarters of overdose victims reported at least one post-overdose morbidity symptom, including pneumonia, palsy, rhabdomyolysis, pulmonary edema, seizure, or cardiac arrhythmia (Warner-Smith, Darke, & Twenty-four hour period, 2002). Studies have also documented low among opioid overdose victims, but the lack of baseline assessments limit identification of significant associations between depression and overdose (Dassanyake et al., 2012). Corrigan & colleagues (2013) withal suggest that diminished performance in several cognitive domains can increase depressive symptoms and negatively impact everyday functioning and the likelihood of poorer social and vocational outcomes.
Opioid-Induced Respiratory Depression
Non-fatal overdose is associated with a number of postal service-overdose complications. Opioid-induced respiratory depression (OIRD) is identified as a primary complexity and the near dangerous source of agin health outcomes associated with NFOO (Rex, Morris, & Schahmann, 2015). OIRD is caused by the activation of the µ-opioid receptor (MOR) expressed on the surface of neurons in brainstem respiratory centers that control breathing (Dahan et al., 2018). In almost NFOO cases, OIRD appears in the grade of acute respiratory compromise with the victim reverting to normal breathing activeness, either on their ain or with the apply of an opioid antagonist like naloxone (Wermeling, 2015). Near NFOO victims recover from acute OIRD and present pocket-size health consequences lasting minutes to hours (Sporer & Dorn, 2001; Buajordet et al., 2004; Olfson et al., 2018).
In some cases, such as when higher dose opioids are consumed or when opioids are taken concurrently with other key nervous system (CNS) depressants (e.g., benzodiazepine), acute respiratory compromise can progress into respiratory distress, abeyance of animate (i.e., apnea), cardiorespiratory collapse, respiratory arrest, and decease (Solis et al., 2017; Dassanayake & Michie, 2012). Enquiry indicates that enduring cognitive and physical consequences are associated with NFOO as OIRD progresses from irregular animate to apnea to the protracted loss of oxygen (Quinn & Abbot, 2014). Hypoxia-related outcomes associated with opioid poisoning include kidney failure, heart complications, neurologic consequences, seizures, nervus damage, temporary motor paralysis, fluid buildup in the lungs, stroke, and pneumonia from inhaling vomitus (Marino et al., 2018; Betts, Ritter, & Kubal, 2012; O'Brien & Todd, 2009; Fitzgerald et al., 2000).
Encephalon Injury
The health consequences of OIRD associated with NFOO include a range of acute complications that develop during and/or immediately after an overdose event. Relatively deficient is literature detailing the more chronic health outcomes that develop among victims experiencing ane or more than NFOO. The majority of chronic literature concerns the development of hypoxic-related encephalon injuries associated with NFOO and subsequent complications (Ueno et al., 2018; Somerville et al., 2017; Betts, Ritter, & Kubal, 2012; Salazar & Dubow, 2012). The hippocampus, basal ganglia, and globous pallidus seem peculiarly susceptible to injury, with short-term memory loss and changes in cognitive and physical functioning indicated as symptomatic outcomes. Stroke has been observed in rare NFOO cases and secondary infections from injecting opioids (due east.thou., endocarditis) tin lead to brain abscesses or meningitis, further extending the injury. Opioid-induced, hypoxic brain injury tin as well lead to the evolution of sever disability, including mental disorientation, ataxia, gait disturbances, incontinence, paraplegia, and catatonia, among a range of other presentations (Buttner et al., 2000). Slower reaction time, impaired memory (amnestic syndrome), reduced motor skills, and diminished physical functioning have all been documented with hypoxic brain injuries associated with NFOO (Barash, Somerville, & DeMaria, 2017; Ueno et al., 2018; Somerville et al., 2017; Betts, Ritter, & Kubal, 2012; Salazar & Dubow, 2012). More than notable is one study indicating the increased run a risk for hypoxic brain impairment among persons who feel multiple or recurring opioid overdose events due to repeated and prolonged hypoxia (Zamora et al., 2015).
Episodes of delayed post-hypoxic leukoencephalopathy--a rare type of neuron damage caused past a prolonged flow of oxygen deficiency--are documented among overdose victims and indicated via MRI by slight deterioration of the periventricular regions of the brain. A contempo Morbidity and Mortality Weekly Report (MMWR) documented a cluster of cases of sudden onset amnesia, a rare cause of memory loss often associated with toxic exposure (due east.g., carbon monoxide poisoning), in Massachusetts between 2012 and 2022 (Barash, Somerville, & DeMaria, 2017). These cases were similarly confirmed by MRI and involved acute and complete ischemia (i.e., a restriction in blood supply to tissues that cause a shortage of oxygen) of both hippocampi. The cause of the acute amnesia amid these patients is unknown to researchers, just the toxicological presence of opioids beyond cases suggests associations with substance utilise.
Differences in Effects of Overdoses between Single, Multiple, and Recurring Opioid Overdose
Differential wellness complications associated with single, multiple, and recurring opioid overdose were identified. Near notable is the identification of a strong correlation between prior and future NFOO events, as persons experiencing a single NFOO event were found more likely to experience a future overdose event in their lifetime; ergo, a person's overdose risk increases with every overdose they experience (Olfson et al., 2018; Darke et al., 2014). NFOO victims who experience multiple/recurring opioid overdose are shown to be at greater risk for long-term physical and cerebral consequences resulting from OIRD than persons experiencing a single overdose. (Darke et al., 2007). Repeatedly subjecting the brain to a deficiency of oxygen is shown to cause damage to the white matter of the brain (King, Morris, & Schahmann, 2015), and the gamble for neurophysiological consequences increases with the both number of times a person experiences a hypoxic/anoxic event and the duration of each result (Beeskow et al., 2018).
3.2. Differing Wellness Outcomes between Illicitly-Manufactured Fentanyl, Heroin, and Prescription Opioids
Studies included in this review have identified the overdose risks associated with opioid analgesics via their interaction with the MOR and the depressive upshot on the CNS. The synthetic opioid fentanyl stands apart from heroin and other semi-synthetic opioids in these findings past its high potency relative to heroin--fentanyl is 50x more strong past weight than heroin--and its rapid onset of action (v-10 seconds when injected), both of which are made possible because of fentanyl'due south loftier lipophilicity and its power to rapidly cross the blood-brain barrier (Burns et al., 2016). The number of fatal IMF-involved overdoses has increased substantially since 2013, surpassing the number of deaths from heroin and prescription opioids in 2022 and 2017, with a 45.2% change in Imf-involved overdose deaths from 2016-2017 (19,413-28,466, respectively; Scholl et al., 2019). Few studies, however, have examined whether there are specific health complications associated with Imf-involved overdose compared to overdoses involving prescription opioids or heroin.
While the epidemiological literature on overdose-related wellness outcomes linked to International monetary fund are negligible (Somerville et al., 2017), the medical research literature does place several iatrogenic side effects (i.eastward., side effects resulting from medical treatment) associated with the clinical apply of intravenous fentanyl in hospital settings, specifically skeletal muscle rigidity and chest wall rigidity (Burns et al., 2016). Breast wall rigidity, colloquially referred to as "wooden chest syndrome," is understood as the acute inability to ventilate or motility the breast wall. Wooden chest syndrome presents obstacles for reversing respiratory depression associated with fentanyl toxicity, due to the hardening of the chest wall and the inability to ventilate victims, but the syndrome is shown to dissipate with naloxone administration. Rigid chest is not commonly associated with natural and semi-synthetic opioids and mainly observed in the synthetic lipid soluble compounds (e.m., fentanyl, acetyl fentanyl and sufentanil).[vii] Because fentanyl is known to produce sudden respiratory consequences at toxic levels, the potential for rapid respiratory depression and arrest may illustrate potential risks for reversing overdoses involving International monetary fund in street settings given reports of sudden unresponsiveness and rapid onset hypoxia associated with IMF (Somerville et al., 2017; MMWR).
Solis, Cameron-Burr, & Kiyatkin (2017) also studied differences between heroin, fentanyl, and fentanyl-adulterated heroin and each substance's influence on factors associated with respiratory low leading to acute hypoxia in rats. They establish that while all 3 heroin/heroin+fentanyl configurations led to decreased oxygen concentrations in rats, fentanyl caused a faster drop in oxygen levels than heroin, and heroin-containing fentanyl led to more than sustained hypoxia and greater decreases in body temperature than both heroin and fentanyl lone. Ii additional example studies also examined differences in wellness outcomes for NFOO involving fentanyl compared to heroin and other opioids, with both studies describing episodes of delayed postal service-hypoxic leukoencephalopathy[8] after a NFOO involving fentanyl (Beeskow et al., 2018; Betts, Ritter, & Kubal, 2012). In both case studies, patients experienced symptoms of mail-hypoxic leukoencephalopathy about 3 weeks after a non-fatal overdose; for both patients, these symptoms included odd behavior, agitation, and decreased psychomotor or cognitive activity, equally well as retentiveness impairment in one of the patients (Beeskow et al., 2018; Betts et al., 2012). While neither case written report described the full recovery of patients, one study did demonstrate patient comeback at 6-months (Betts et al., 2012).
3.3. Interaction between Pre-existing Weather condition and Subsequent Overdose
As with the differences in outcomes between Imf and other opioid-related not-fatal overdoses, few studies take examined the coaction between already-existing physical or mental weather and subsequent NFOO. Some mental health conditions, such as depression and suicidality, have been strongly associated with opioid use disorder and drug overdose. Comorbid mental health conditions are identified every bit take chances factors for drug overdose but it is difficult to distinguish the degree to which they are influenced or exasperated by NFOOs in retrospective studies (Neale, 2000). Tobin & Latkin (2003), for example, found that individuals who had experienced an overdose within 12 months prior to being interviewed scored significantly higher on low indexes compared to those that had not. In this case, depression may have acted as a catalyst for the overdose result, been exasperated by it, or both. Beyond depression, intentional suicide attempts are shown to be associated with unintentional overdose (Neale, 2000; Bradvick et al., 2007), with intentional suicide run a risk correlated with a college number of drug overdoses (Bradvick et al., 2007). It is unclear, however, to what degree suicidality is exasperated past drug overdose.
A similar interplay is described with respect to prefrontal cortex functioning and opioid misuse and abuse. According to the cognitive deficits model, concrete abnormalities in the construction of the prefrontal cortex tin make information technology more difficult for individuals to command their impulses and drug employ behavior. As individuals succumb to their impulses and utilize opioids and overdose, hypoxia can event in damage to the prefrontal cortex, worsening their addiction and increasing negative cerebral and mental health outcomes (Kosten & George, 2002).
Symptoms associated with the opioid overdose-induced hypoxic injuries described above may exasperate already-existing disabilities and conditions. Barash & colleagues (2017), for case, documented three cases of seizures associated with opioid overdose: 1 had previously experienced seizures, ane experienced seizure during their acute overdose, and one developed a seizure disorder and post-overdose amnesia. While researchers did not certificate a history of worsening epilepsy, they were able to show an interaction between seizures and opioid overdose at each stage. Accordingly, declines in cognitive and concrete functioning instigated by NFOO may likewise make it hard for individuals to manage their existing chronic illnesses, such as diabetes and clinical low (King, 2015).
Finally, information technology is possible that the interaction between inability and opioid overdose has non been well examined simply considering some of the health outcomes are rare and hard for physicians and researchers to identify through standard medical do. For example, in one example study, physicians described the claiming of diagnosing a immature woman with a history of seizures and cri du chat, a developmental disability. The medical team focused heavily on characterizing the woman'south altered level of consciousness and ran extensive tests earlier taking a full history with her caregiver and discovering her contempo codeine use (Kumar, 2007).
3.iv. Wellness Service Utilization
Inquiry containing data about utilization of wellness services after a non-fatal overdose is likewise scarce. One study meeting our inclusion/exclusion criteria conducted in Australia approximately 20 years agone found that, within their sample of current heroin users, virtually ane-half had experienced a non-fatal overdose in their lifetime; following these non-fatal overdoses, 54% of respondents were administered naloxone, 59% reported that an ambulance attended the overdose, and 45% of respondents were hospitalized because of the overdose (McGregor et al., 1998).
4. DISCUSSION
4.i. Discussion of Results
Our findings suggest NFOO is associated with the current opioid epidemic and represents an increasing proportion of morbidity in the United States. The electric current and past enquiry on not-fatal opioid overdose included in this review describe a number of physiological complications stemming from an NFOO event. Information technology is notable that the vast bulk of clinical presentations associated with non-fatal opioid overdose identified in the literature are acute complications of the opioid overdose itself, with findings indicating that near consequences appear during or immediately after the overdose event, or in days to weeks subsequently.
Evidence indicates that people who experience a single opioid overdose are more likely to have subsequent overdoses (Dassanyake et al., 2012), and multiple and repeated opioid overdoses are correlated with decreasing cognitive performance (Darke et al., 2007), increases in depression symptoms (Tobin & Latkin, 2003), and suicidal ideation (Bradvick et al., 2007). The findings related to IMF, specifically its event on increasing the cumulative number of overdoses individuals volition experience in a lifetime, raise the possibility that people who repeatedly experience a NFOO may exist undergoing recurrent hypoxic events and experiencing "minor" brain injuries whose negative effects are compounded by repetition. Beyond studies identifying opioid overdose-induced brain injuries via MRI, the recurring onset of hypoxia characteristic of "series overdosers" may generate no immediate symptoms, while others may be and then subtle that it becomes difficult for people to recognize, or symptoms may not announced for weeks, months, or years after. Consequently, these findings illustrate a plausible parallel between concussions as a traumatic brain injury on the one hand and opioid overdose-related hypoxic events as a "milder" encephalon injury on the other: both events touch on the brain and both are known to exist associated with physical, mental, and cognitive complications.
Sharp increases in Imf supply and consumption since 2013 take been linked to the abrupt rise in fentanyl-involved overdoses, with the number of fentanyl overdoses surpassing the number of prescription opioid and heroin overdoses for 2022 and 2022 (DEA, 2018). Fentanyl is a highly potent synthetic opioid that is roughly 50 times more potent by weight than heroin (Wade et al., 2015). Increased fentanyl consumption has given ascension to the panoply of acute health complications described above, simply numerous reports besides indicate that Imf is engendering unique and heretofore uncommon overdose presentations non seen with natural and semi-synthetic opioids (Somerville et al., 2017). A recent study in rats detected rapidly stiff but transient decreases in extracellular oxygen levels when human being-relevant doses (twoscore mcg/kg) of fentanyl was administered, with brain hypoxic effects condign significantly enhanced when the fentanyl dose increased by x% (Solis, Cameron-Burr, & Kiyatkin, 2017). As with similar pharmacokinetic studies on fentanyl toxicity, these findings indicate that illicit fentanyl consumption, fifty-fifty in nominal amounts, poses heightened risks for acute brain complications, including enhanced brain hypoxia and induced brain hypothermia. Additional symptoms associated with fentanyl toxicity have as well been documented, including sudden respiratory distress, rigor mortis, rigid breast, comatose, immediate cyanosis, amongst others (Somerville et al., 2017; Burns et al., 2016).
The surge in Imf consumption has not only contributed to concurrent increases in International monetary fund-involved overdoses (as noted by a recent CDC report indicating a 45% increase in fentanyl-involved deaths from 2016-2017) just the cumulative number of overdoses experienced by individuals are also increasing (Scholl et al., 2019). An increase in the number of lifetime overdoses experienced by people using Imf is peculiarly disconcerting given the impairment that recurring hypoxic[9] and anoxic events[ten] can have on the brain. At present, there are effective, testify-based interventions that can reduce the negative health effects associated with NFOO, such equally training and equipping opioid consumers, emergency responders, bystanders, family unit members, correctional officers, and drug treatment and health care providers in the use of naloxone (Beletsky, 2012). Naloxone, a drug that counters the effects of opioids, is constructive in temporarily reversing the depressive effects of an opioid overdose (U.S. Surgeon General, 2018) and reducing opioid overdose death rates (McClellan et al., 2018). The rapid onset of respiratory depression and abort associated with acute fentanyl toxicity makes the risk of hypoxic and anoxic events more likely, suggesting that naloxone may demand to be administered more than chop-chop than overdoses involving other opioids, in addition to potentially needing more than one dose per overdose reversal.
4.2. Gaps in the Literature
Our review of the literature identified several knowledge gaps. Specifically, while acute complications that transpire during or shortly later an opioid overdose are detailed and robust, the paucity of findings on the chronic complications resulting from recurring non-fatal opioid overdose events are alarming given the evidence nosotros do have on hypoxic brain injuries stemming from opioid-induced toxicity. In addition, given what we know about fentanyl's dominance and the surge in IMF-involved overdoses, the limited number of publications examining differences in health outcomes between heroin, Imf, and prescription opioids was surprising. The current literature suggests that non-fatal overdoses involving synthetic opioids (east.one thousand., fentanyl) can lead to more serious or longer-term health outcomes, only the specific discrepancies between health outcomes involving these types of drugs has still to exist examined more than in-depth. A gap as well appears to exist on whether existing concrete and mental health outcomes among persons who misuse and corruption opioids become exacerbated when said consumers feel (>1) non-fatal opioid overdose. This lack of data is compounded by the retrospective blueprint of many studies, which makes rigorously evaluating the functional status of individuals prior to overdose exceptionally challenging. The electric current famine of longitudinal studies examining these topics restricts our power to understand the myriad complications of opioid overdose on victims' physical, mental, and cognitive operation, and specifically the downstream effects of a fentanyl overdose crisis that, at present, involves thousands of people.
4.3. Importance of Information
As the number of non-fatal opioid-involved opioids continues to grow, information technology is paramount that health care and treatment providers as well as policymakers accept information on the wellness and functional outcomes of individuals who have experienced singular, multiple, or reoccurring overdose events. This is especially true of IMF-involved overdoses. Without this information, providers and policymakers will be hindered in their ability to provide appropriate and loftier-quality health care and supportive services for individuals who take experienced 1 or multiple overdose events. However, our review demonstrated that in that location is a paucity of peer-reviewed and grey publications leaving gaps in our agreement of the health and functional outcomes of non-fatal opioid overdoses. Further inquiry that includes an boosted review of the literature with expanded search strategies, the drove of primary information through interviews, and longitudinal studies utilizing secondary data, may address these knowledge gaps.
4.4. Study Limitations
Although our review yielded many studies presenting acute health consequences of an overdose, few focused on the chronic wellness and functional outcomes of not-fatal overdoses. Too, there appears to exist piddling information in the peer-reviewed or grey literature regarding the differences in short-term and long-term health and functional outcomes between Imf and semi-constructed opioids. Similarly, our review institute very few publications that examined the interplay between pre-existing conditions and non-fatal overdose.
It is unclear if the limited number of publications examining these topics is truly a reflection of the amount of research currently being conducted in this expanse or a reflection of the limitation in our search criteria. Although our squad included a senior librarian and multiple (three) separate searches of the peer-reviewed literature and a thorough review of the greyness literature, our review may have been express past our search terms. For example, several publications were non identified in the first endeavour in the peer-reviewed literature because they did not include the terms (or variations) of "opioid," "overdose," or "non-fatal" in their titles or keywords. Time to come reviews should build upon our search strategy and aggrandize the listing of search terms to include specific names of medications and health outcomes known to be associated with not-fatal overdose.
5. Decision
The purpose of this scoping review was to better understand wellness and functional outcomes associated with NFOO. After reviewing 48 peer-reviewed and gray publications identified and selected for review, our analysis concluded that numerous clinical complications are associated with non-fatal opioid overdose. Among these, most focus on astute outcomes stemming from respiratory depression and related hypoxia.
Epidemiological enquiry suggests that the increased saturation of International monetary fund in existing heroin markets may be serving every bit an overdose risk modifier due to fentanyl's pharmacokinetics as a synthetic opioid and its higher dominance compared to heroin (Dragoovic, Tamburro & Hadidi, 2016; Marinetti & Ehlers, 2014). IMF is contributing to a rise in severe and uncommon opioid overdose presentations and increasing the cumulative number of overdose events experienced by individual fentanyl consumers. The combination of atypical overdose complications on the one hand and cumulative increases in the number of overdose events on the other raises concerns that recurring hypoxic brain injuries experienced by overdose victims may be contributing to chronic brain damage and associated physical, mental, and cerebral disability among this population.
Taken together, these findings raise the possibility that people who repeatedly feel an opioid overdose may be undergoing recurring hypoxic events and experiencing "pocket-size" brain injuries whose effects may exist compounded by repetition. This hypothesis is based on same findings whose evidence points to a plausible parallel betwixt recurring overdose events and echo concussions, with opioid overdose-induced hypoxia understood equally a "milder" grade of encephalon injury: concussions and hypoxic overdose events both affect the encephalon, and both are associated with diseases that bear upon the function or structure of the brain.
The electric current dearth of longitudinal studies examining the more than chronic complications resulting from multiple or recurring non-fatal opioid overdose events restricts our ability to understand the longer-term effects of opioid overdose on victims' physical, mental, and cognitive operation, which is compounded by the unknown downstream furnishings of a fentanyl overdose crisis that, at present, involves hundreds of thousands of people. Although the studies examined as part of this scoping review do offer insight into the myriad consequences of non-fatal opioid overdose on victims' concrete and mental health, large gaps in our noesis of NFOO still exist. Potentially fruitful avenues for future research include an additional review of the NFOO literature with expanded search strategies, the drove of primary data through interviews with key subject affair experts and NFOO victims, and longitudinal cohort studies that follow overdose victims for decades. A longer-term recommendation for clinical research may even include expanding current encephalon injury studies, such as the Chronic Traumatic Encephalopathy Program at Boston University, to include brains of fatal overdose victims who are known to have experienced--and/or been negatively affected by--repeated non-fatal hypoxic overdose events prior to expiry.
REFERENCES
Arksey, H., & O'Malley, 50. (2005). Scoping studies: towards a methodological framework. International Journal of Social Research Methodology, 8, xix-32.
Baca, C.T., & Grant, 1000.J. (2005). Take-home naloxone to reduce heroin death. Addiction, 100(12), 1823-1831.
Bachi, K., Sierra, S., Volkow, N.D., Goldstein, R.Z., & Alia-Klein, N. (2017). Is biological aging accelerated in drug addiction? Curr Opin Behav Sci, xiii, 34-39.
Barash, J.A., Somerville, N., & DeMaria, A. Jr. (2017). Cluster of an unusual amnestic syndrome--Massachusetts, 2012-2016. MMWR, 66(3), 76. Retrieved from https://www.cdc.gov/mmwr/volumes/66/wr/mm6603a2.htm.
Beeskow, A.B., Oberstadt, Thousand., Saur, D., Hoffman, K.T., & Lobsien, D. (2018). Delayed post-hypoxic leukoencephalopathy (DPHL)--An uncommon variant of hypoxic encephalon damage in adults. Frontiers in Neurology, 9.
Beletsky, Fifty., Rich, J.D., & Walley, A.Y. (2012). Prevention of fatal opioid overdose. JAMA, 308(eighteen), 1863-1864.
Betts, A.Chiliad., Ritter, J.50., & Kubal, W.S. (2012). Reversible delayed posthypoxic leukoencephalopathy after drug overdose: MRI findings in a drove of patients. Emergency Radiology, nineteen(2), 165-173.
Bail, G.R., Ho, 1000., & Woodward, R.W. (2012). Trends in hepatic injury associated with unintentional overdose of paracetamol (acetaminophen) in products with and without opioid: An assay using the National Toxicant Data Organization of the American Association of Poison Command Centers, 2000-7. Drug Prophylactic, 35(two), 149-157.
Bradvik, L., Frank, A., Hulenvik, P., Medvedeo, A., & Berglund, 1000. (2007). Heroin addicts reporting previous heroin overdoses also study suicide attempts. Suicide Life Threat Behav, 37(four), 475-81.
Buajordet, I., Naess, A.C., Jacobsen, D., & Brørs, O. (2004). Adverse events after naloxone treatment of episodes of suspected acute opioid overdose. Eur J Emerg Med, 11(1), 19-23.
Burns Thou., DeRienz R.T., Baker D.D., Casavant 1000., & Spiller H.A. (2016). Could breast wall rigidity be a factor in rapid death from illicit fentanyl abuse? Clin Toxicol (Phila), 54(v), 420-423.
Buttner, A., Mall, Chiliad., Penning, R., & Weis, Southward. (2000). The neuropathy of heroin abuse. Forensic Science International, 113, 435-442.
CDC. (2018). Vital signs: Trends in emergency department visits for suspected opioid overdoses--United States, July 2016-September 2017. MMWR, 67(9), 279-285.
CDC. (2017). Almanac surveillance report of drug-related risks and outcomes--United States, 2017. Atlanta, GA: U.S. Department of Wellness and Human Services, CDC. Retrieved from: https://www.cdc.gov/drugoverdose/pdf/pubs/2017-cdc-drug-surveillance-study.pdf.
CDC. (2016). Wide-ranging online data for epidemiologic research (WONDER). Atlanta, GA: U.S. Department of Health and Human Services, CDC, National Heart for Wellness Statistics. Retrieved from: https://wonder.cdc.gov.
Coffin, P.O., Tracy, 1000., Bucciarelli, A., Ompad, D., Vlahov, D., & Galea, Due south. (2007). Identifying injection drug users at risk of nonfatal overdose. Acad Emerg Med, 14(7), 616-623.
Colquhoun, H.Fifty., Level, D., O'Brien, K.K., Straus, Due south., Tricco, A.C., Perrier, L., Kastner, Thou., & Moher, D. (2014), Scoping reviews: Time for clarity in definition, methods, and reporting. Journal of Clinical Epidemiology, 67(12), 1291-1294.
Conner, Yard.R., Britton, P.C., Sworts, L.M., & Joiner, T.E. Jr. (2007). Suicide attempts amidst individuals with opiate dependence: The critical role of belonging. Aficionado Behav, 32(vii), 1395-1404.
Darke, S., Marel, C., Mills, K.L., Ross, J., Slade, T., Burns, L. & Tesson, Chiliad. (2014). Patterns and correlates of non-fatal heroin overdose at 11-year follow-up: Findings from the Australian Handling Event Study. Drug Booze Depend, 144, 148-152.
Darke, S., Sims, J., McDonald, S., & Wickes, Due west. (2000). Cognitive impairment among methadone maintenance patients. Addiction, 95(v), 687-695.
Darke, S., Williamson, A., Ross, J., Mills, K.Fifty., Harvard, A., & Teesson, One thousand. (2007). Patterns of nonfatal heroin overdose over a iii-year period: Findings from the Australian treatment effect study. J Urban Health, 84(ii), 283-291.
Darke, S., Williamson, A., Ross, J., & Teesson, M. (2005). Non-fatal heroin overdose, treatment exposure and customer characteristics: Findings from the Australian treatment event study (ATOS). Drug Alcohol Rev, 24(five), 425-432.
Dassanayake, T.L., Michie, P.T., Jones, A., Carter, G., Mallard, T., & Whyte, I. (2012). Cerebral impairment in patients clinically recovered from central nervous system depressant drug overdose. Journal of Clinical Psychopharmacology, 32(4), 503-510.
Dragovic, L., Tamburro, 50., & Al-Hadidi, J. (2016). Resurgence of fentanyl as a drug of abuse. Journal of Forensic Science & Medicine, 2(2), 111-114.
Duru, U.B., Pawar, M., Barash, J.A., Miller, L.Due east., Thiruselvam, I.K., & Haut, M.W. (2018). An unusual amnestic syndrome associated with combined fentanyl and cocaine use. Ann Inter Med, 168(10), 747-748
Elmer, J., Flickinger, K.Fifty., Anderson, M.W., Koller, A.C., Sundermann, G.50., Dezfulian, C., Okonkwo, D.O., Shutter, L.A., Salcido, D.D., Callaway, C.W. & Menegazzi, J.J. (2018). Outcome of neuromonitor-guided titrated care on brain tissue hypoxia after opioid overdose cardiac abort. Resuscitation, 129, 121-126.
Ersche, Yard.D., & Sahakian, B.J. (2007). The neuropsychology of amphetamine and opiate dependence: Implications for handling. Neuropsychology Review, 17(3), pp. 317-336.
Fitzgerald, J., Hamilton, M., & Dietze, P. (2000). Walking overdoses: A re-appraisement of non-fatal illicit drug overdose. Addiction Research, 8(4), 327-355.
Hantson, P., Vanbinst, R., & Wallemacq, P. (2003). Accidental methadone overdose in an opiate-naive elderly patient. Intensive Care Medicine, 29(xi), 2105.
Havens, J.R., Oscer, C.B., Knudsen, H.K., Lofwall, Grand., Stoops, Westward.West., Walsh, S.Fifty., Leukefeld, C.Grand., & Kral, A. (2011). Individual and network factors associated with non-fatal overdose amongst rural Appalachian drug users. Drug & Alcohol Dependence, 115, 107-112.
Heale, P., Dietze, P., & Fry, C. (2003). Intentional overdose amid heroin overdose survivors. J Urban Health, 80(ii), 230-237.
Hedegaard, H., Warner, M., & Miniño, A.M. (2017). Drug overdose deaths in the United states, 1999-2016. NCHS data brief, no 294. Hyattsville, MD: U.South. Department of Health and Homo Services, CDC, National Center for Health Statistics. Retrieved from: https://www.cdc.gov/nchs/data/databriefs/db294.pdf.
King, F., Morris, N.A., & Schahmann, J.D. (2015). Delayed post-hypoxic leukoencephalopathy: Improvement with antioxidant therapy. Example Reports in Neurology, 7, 242-246.
Kumar, A. (2007). Adventitious iatrogenic opioid overdose: A difficult diagnosis. British Periodical of Anaesthetic & Recovery Nursing, 8(1), 5-vi.
Kumar, N., Bhalla, M.C., Frey, J.A., & Southern, A. (2015). Intraparenchymal hemorrhage after heroin use. American Journal of Emergency Medicine, 33(viii), 1109.e3-1109.e4.
Levac, D., Colquhoun, H., & O'Brien, Thousand.1000. (2010). Scoping studies: Advancing the methodology. Implementation Scientific discipline, five(69), 1-nine.
Marinetti, 50.J., & Ehlers, B.J. (2014). A series of forensic toxicology and drug seizure cases involving illicit fentanyl alone and in combination with heroin, cocaine or heroin and cocaine. Journal of Analytical Toxicology, 38(8), 592-598.
McClellan, C., Lambdin, B.H., Ali, 1000.M., Mutter, R., Davis, C.South., Wheeler, E., Pemberton, Thousand., & Kral, A.H. (2018). Opioid-overdose laws association with opioid use and overdose mortality. Addictive Behaviors, 86, ninety-95.
McGregor, C., Darke, South., Ali, R., & Christie, P. (1998). Experience of non-fatal overdose amidst heroin users in Adelaide, Australia: Circumstances and take a chance perceptions. Addiction, 93(v), 701-711.
Mulpur, A.M., Mirsadraee, Southward., Hassan, T.B., McKeague, H., & Kaul, P. (2004). Refractory ventricular fibrillation in accidental hypothermia: Salvage with cardiopulmonary bypass. Perfusion, 19(5), 311-314.
Neale, J. (2000). Suicidal intent in non-fatal illicit drug overdose. Addiction, 95(1), 85-93.
O'Donnell, J.K., Gladden, R.One thousand., & Seth, P. (2017). Trends in deaths involving heroin and constructed opioids excluding methadone, and law enforcement drug product reports, by census region--United states of america, 2006-2015. MMWR, 66(34), 897-903. Retrieved from: https://www.cdc.gov/mmwr/volumes/66/wr/mm6634a2.htm.
Olfson, Grand., Crystal, S., Wall, M.Thousand., Wang, S., Liu, S.M., & Blanco, C. (2018). Causes of death after nonfatal opioid overdose. JAMA Psychiatry, 75(8), 820-827.
National Institutes of Health (NIH). (n.d.). Opioid overdose crunch, Retrieved from: https://world wide web.drugabuse.gov/drugs-abuse/opioids/opioid-overdose-crunch.
Paulozzi, L.J., Zhang, Thou., Jones, C.M., & Mack, K.A. (2014). Hazard of adverse health outcomes with increasing duration and regularity of opioid therapy. JABFM, 27(iii), 329-338.
Pfab, R., Eyer, F., Jetzinger, Due east., & Zilker, T. (2006). Cause and motivation in cases of not-fatal drug overdoses in opiate addicts. Clin Toxicol (Phila), 44(iii), 255-259.
Quinn, D.K., & Abbott, C.C. (2014). Catatonia subsequently cerebral hypoxia: Practice the usual treatments apply? Psychosomatics, 55(6), 525-535.
Reece, A., & Hulse, G. (2013). Lifetime opiate exposure as an independent and interactive cardiovascular risk cistron in males: A cantankerous-sectional clinical report. Vasc Health Risk Manag, nine, 551-561.
Ridgeway, Z.A., & Pountney, A.J. (2007). Acute respiratory distress syndrome induced by oral methadone managed with not-invasive ventilation. Emerg Med J, 24(9), 681.
Salazar, R., & Dubow, J. (2012). Delayed pothypoxic leukoencephalopathy following a morphine overdose. Journal of Clinical Neuroscience, 19, pp. 1060-1062.
Scholl, Fifty., Seth, P., Kariisa, M., Wilson, Northward., & Baldwin, K. (2019). Drug and opioid-involved overdose deaths--United States, 2013-2017. MMWR, 67(5152), 1419-1427. Retrieved from: https://world wide web.cdc.gov/mmwr/volumes/67/wr/mm675152e1.htm.
Solis, E. Jr., Cameron-Burr, K.T., & Kiyatkin, E.A. (2017). Heroin contaminated with fentanyl dramatically enhances encephalon hypoxia and induces brain hypothermia. eNeuro, 4(5), pp. 1-10.
Somerville N.J., O'Donnell, J., Gladden, R.M., Zibbell, J.Due east., Green, T.C., Younkin, M., Ruiz, S., Babakhanlou-Chase, H., Chan, M., Callis, B.P., Kuramoto-Crawford, J. Nields, H.K., & Walley, A.Y. (2017). Characteristics of fentanyl overdose--Massachusetts, 2014-2016. MMWR, 66, 382-386
Sporer, K.A., & Dorn, E. (2001). Heroin-related noncardiogenic pulmonary edema--A case series. Breast, 120(v), 1628-1632.
Stewart, D., Gossop, Chiliad., & Marsden, J. (2002). Reductions in not-fatal overdose after drug misuse treatment: Results from the National Treatment Outcome Research Study (NTORS). Journal of Substance Abuse Treatment, 22(i), 1-ix.
Tobin, K.East., & Latkin, C.A. (2003). The relationship between depressive symptoms and nonfatal overdose among a sample of drug users in Baltimore, Maryland. J Urban Wellness, 80(2), 220-229.
U.S. Section of Justice, Drug Enforcement Administration (DEA). (2018). 2022 National Drug Threat Assessment. Retrieved from: https://www.dea.gov/sites/default/files/2018-eleven/DIR-032-18%202018%20NDTA%20final%20low%20resolution.pdf.
U.S. Surgeon General. (2018). Surgeon General's Advisory on Naloxone and Opioid Overdose. Retrieved from: https://world wide web.surgeongeneral.gov/priorities/opioid-overdose-prevention/naloxone-advisory.html.
Warner-Smith, M., Darke, S., & Twenty-four hour period, C. (2002). Morbidity associated with nonfatal heroin overdose. Addiction, 97(viii), 963-967.
Warner-Smith, K., Darke, S., Lynskey, M., & Hall, W. (2001). Heroin overdose: Causes and consequences. Addiction, 96(eight), 1113-1125.
Wermeling, D.P. (2015). Review of naloxone safety for opioid overdose: Practical considerations for new technology and expanded public access. Ther Adv Drug Saf, 6(1), 20-31.
Wines, J.D. Jr., Saitz, R., Horton, N.J., Lloyd-Travaglini, C., & Samet, J.H. (2007). Overdose after detoxification: A prospective study. Drug Alcohol Depend, 89(2-iii), 161-169.
Yen, Y.F., Chou, P., Lin, Y.S., & Deng, C.Y. (2015). Factors associated with health-related quality of life among injection drug users at methadone clinics in Taipei, Taiwan. Journal of the Chinese Medical Association, 78(5), 292-298.
APPENDIX A. EXAMPLE SEARCH STRATEGY--PubMed
PubMed--Search 1
#3 Add Search ((#1 OR #ii) NOT ("Comment"[Publication Type] OR "Alphabetic character"[Publication Type] OR "Editorial"[Publication Type])) Filters: Publication appointment from 1998/01/01; English language 238
#2 Add Search (opioid*[Title] OR fentanyl[Title] OR "illicitly-manufactured fentanyl"[Text Give-and-take] OR "illicitly-made fentanyl"[Text Give-and-take] OR acetylfentanyl[Title] OR furanylfentanyl[Championship] OR carfentanil[Title] OR heroin[Title] OR oxycodone[Title] OR oxymorphone[Championship] OR Opana[Title] OR hydromorphone[Championship] OR Dilaudid[Title] OR OxyContin[Title] OR hydrocodone[Title] OR Vicodin[Title] OR novel psychoactive substance*[Text Word] OR methadone[Title] OR "Analgesics, Opioid"[Mesh] OR "Analgesics, Opioid"[Pharmacological Action] OR "Opioid-Related Disorders"[Mesh] OR "Fentanyl"[Mesh] OR "carfentanil"[Supplementary Concept] OR "Due north-(1-phenethylpiperidin-4-yl)-Northward-phenylacetamide"[Supplementary Concept] OR "Heroin"[Mesh] OR "Heroin Dependence"[Mesh] OR "Oxycodone"[Mesh] OR "Oxymorphone"[Mesh] OR "Hydromorphone"[Mesh] OR "Methadone"[Mesh]) AND (non fatal overdos*[Text Word] OR nonfatal overdos*[Text Word] OR unintentional overdos*[Text Word] OR accidental overdos*[Text Word]) Filters: Publication date from 1998/01/01; English language 202
#1 Add Search (opioid*[Title] OR fentanyl[Title] OR "illicitly-manufactured fentanyl"[Text Word] OR "illicitly-made fentanyl"[Text Word] OR acetylfentanyl[Title] OR furanylfentanyl[Title] OR carfentanil[Championship] OR heroin[Title] OR oxycodone[Title] OR oxymorphone[Title] OR Opana[Title] OR hydromorphone[Title] OR Dilaudid[Title] OR OxyContin[Title] OR hydrocodone[Title] OR Vicodin[Title] OR novel psychoactive substance*[Text Word] OR methadone[Championship] OR "Analgesics, Opioid"[Mesh] OR "Analgesics, Opioid"[Pharmacological Action] OR "Opioid-Related Disorders"[Mesh] OR "Fentanyl"[Mesh] OR "carfentanil"[Supplementary Concept] OR "N-(1-phenethylpiperidin-4-yl)-N-phenylacetamide"[Supplementary Concept] OR "Heroin"[Mesh] OR "Heroin Dependence"[Mesh] OR "Oxycodone"[Mesh] OR "Oxymorphone"[Mesh] OR "Hydromorphone"[Mesh] OR "Methadone"[Mesh]) AND (overdos*[Title] OR "Drug Overdose"[Mesh]) AND ("not-fatal"[Championship] OR nonfatal[Title] OR unintentional*[Title] OR adventitious*[Title] OR accident[Title]) Filters: Publication date from 1998/01/01; English 122
PubMed--Search 2
#1 Add together Search ((opioid*[Title] OR fentanyl[Title] OR "illicitly-manufactured fentanyl"[Text Word] OR "illicitly-made fentanyl"[Text Word] OR acetylfentanyl[Title] OR furanylfentanyl[Title] OR carfentanil[Title] OR heroin[Title] OR oxycodone[Championship] OR oxymorphone[Title] OR Opana[Championship] OR hydromorphone[Title] OR Dilaudid[Title] OR OxyContin[Championship] OR hydrocodone[Title] OR Vicodin[Championship] OR novel psychoactive substance*[Text Give-and-take] OR methadone[Title] OR "Analgesics, Opioid"[Mesh] OR "Analgesics, Opioid"[Pharmacological Activity] OR "Opioid-Related Disorders"[Mesh] OR "Fentanyl"[Mesh] OR "carfentanil"[Supplementary Concept] OR "N-(1-phenethylpiperidin-iv-yl)-N-phenylacetamide"[Supplementary Concept] OR "Heroin"[Mesh] OR "Heroin Dependence"[Mesh] OR "Oxycodone"[Mesh] OR "Oxymorphone"[Mesh] OR "Hydromorphone"[Mesh] OR "Methadone"[Mesh]) AND (overdos*[ti] OR "Drug Overdose"[Mesh]) AND ("Hypoxia"[Mesh] OR "Hypoxia, Brain"[Mesh] OR "hypoxic hypoxia"[tw] OR "arterial hypoxia" OR "hypoxia"[tw]) Filters: Publication engagement from 1998/01/01; English language 16
PubMed--Search iii
#ii Add Search (("Longitudinal Studies"[Mesh] AND ("Drug Overdose/therapy"[Majr] OR "Opioid-Related Disorders/therapy"[Majr]) Non #i)) Filters: Publication date from 1998/01/01; English language 120
#one Add Search ((opioid*[Championship] OR fentanyl[Title] OR "illicitly-manufactured fentanyl"[Text Word] OR "illicitly-made fentanyl"[Text Word] OR acetylfentanyl[Title] OR furanylfentanyl[Championship] OR carfentanil[Championship] OR heroin[Title] OR oxycodone[Title] OR oxymorphone[Title] OR Opana[Title] OR hydromorphone[Title] OR Dilaudid[Title] OR OxyContin[Title] OR hydrocodone[Title] OR Vicodin[Title] OR novel psychoactive substance*[Text Word] OR methadone[Title] OR "Analgesics, Opioid"[Mesh] OR "Analgesics, Opioid"[Pharmacological Activity] OR "Opioid-Related Disorders"[Mesh] OR "Fentanyl"[Mesh] OR "carfentanil"[Supplementary Concept] OR "N-(1-phenethylpiperidin-4-yl)-North-phenylacetamide"[Supplementary Concept] OR "Heroin"[Mesh] OR "Heroin Dependence"[Mesh] OR "Oxycodone"[Mesh] OR "Oxymorphone"[Mesh] OR "Hydromorphone"[Mesh] OR "Methadone"[Mesh]) AND (overdos*[ti] OR "Drug Overdose"[Mesh]) AND ("Longitudinal Studies"[Mesh] OR "Follow-Upward Studies"[Mesh] OR longitudinal[ti] OR follow-upward[ti])) Filters: Publication date from 1998/01/01; English 70
NOTES
-
IMFs include both fentanyl hydrochloride and fentanyl analogs (e.1000., acetylfentanyl, furanylfentanyl, and carfentanil, etc.).
-
Swelling or an infection of the lungs or large airways.
-
Lung congestion.
-
Inflammation of the lungs.
-
The breakdown of damaged skeletal musculus.
-
Damage to the peripheral nerves, such every bit the hands or feet.
-
Come across Fermaglich (1996) [https://jamanetwork.com/journals/jama/article-abstract/395849] for a clarification of the Parkinsonian furnishings associated with the consumption of illicitly-manufactured meperidine (MPTP [one-methyl-4-phenyl-1,2,3,6-tetrahydropyridine], also a constructed opioid. Several substance users were rendered immobile and speechless following utilize of the drug and were colloquial refer to in the press as "frozen addicts." Clinical observations persuade doctors they are suffering from a pernicious course of Parkinson'southward illness. Confirmation arrives when they are treated with levodopa simply have side effects that limit therapy, returning them to their debilitating frozen states.
-
A neurological relapse after initial recovery from an astute event resulting in the loss of oxygen to the brain.
-
Partial supply of oxygen to the brain, only at low levels that are inadequate to maintain normal brain function.
-
Complete interruption of the supply of oxygen to the brain.
Source: https://aspe.hhs.gov/reports/non-fatal-opioid-overdose-associated-health-outcomes-final-summary-report-0
Postar um comentário for "Inabiliaty to Walk Again After Codeine Overdose"